Crushed
1
View details
A 22-year-old construction worker is brought in by first responders. He was trapped inside a ventilation shaft for ~8 hours, following an accidental fall of ~14 feet. During that time, his body was compressed against the pipes and vent walls.
His medical and surgical histories are unremarkable. He is not on any medications. He drinks 15 to 20 units of alcohol each week, but only after work. He denies being intoxicated at the time of the accident. He does not use recreational drugs.
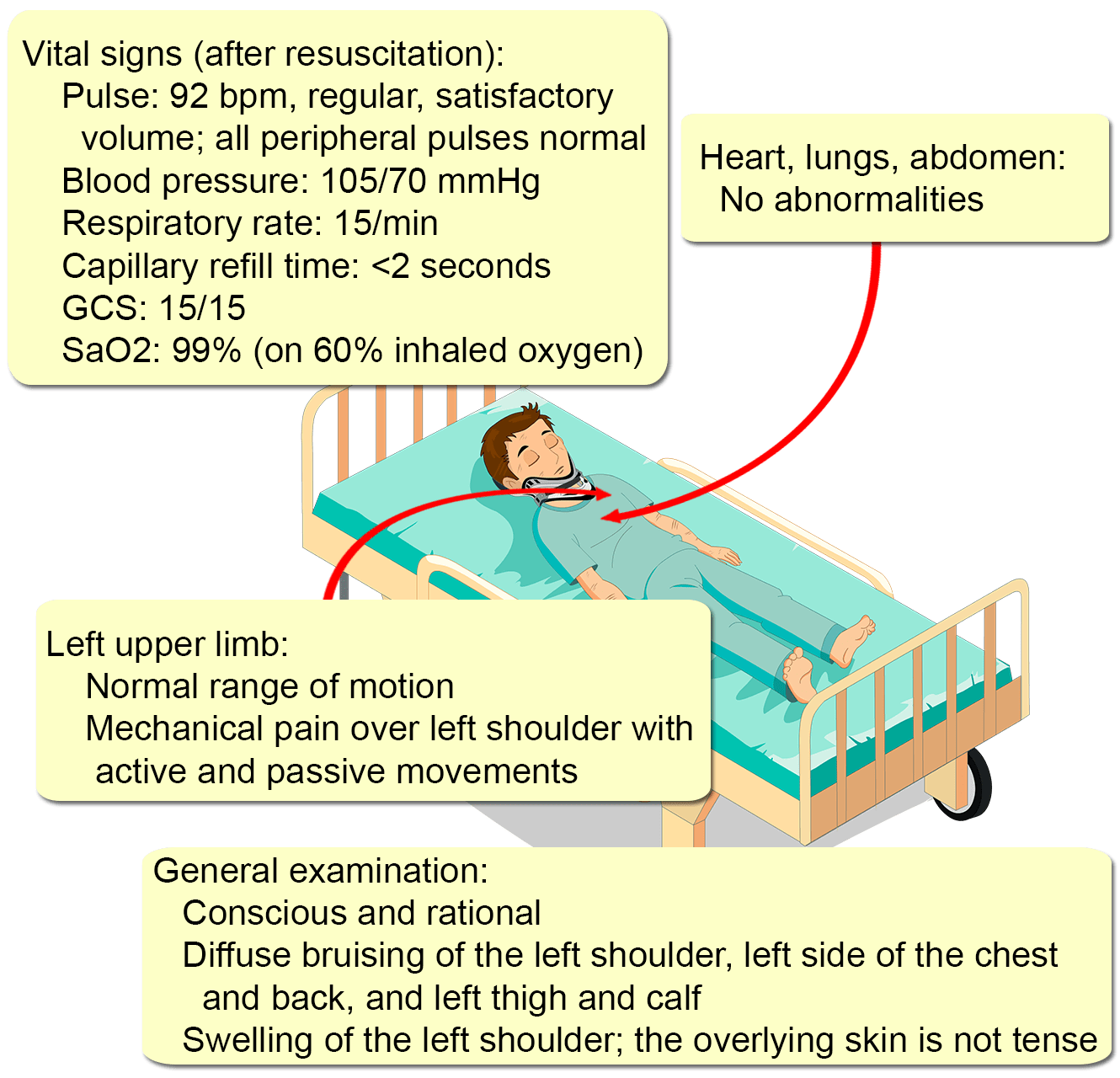
A primary survey is performed. His airway and breathing are unthreatened. However, his pulse is weak, with a rate of 130 bpm. His blood pressure is 70/50 mmHg. Both hands are cold. His GCS is 15/15. Urgent fluid resuscitation is commenced, and his hemodynamic parameters stabilize.
A complete blood count is normal, with a hemoglobin level of 14 g/dL, and hematocrit of 42%. A chest x-ray is normal. An ECG is also normal. A toxicology screen is negative for benzodiazepines, cannabinoids, ethanol, methadone, or opiates.