Excitable
1
View details
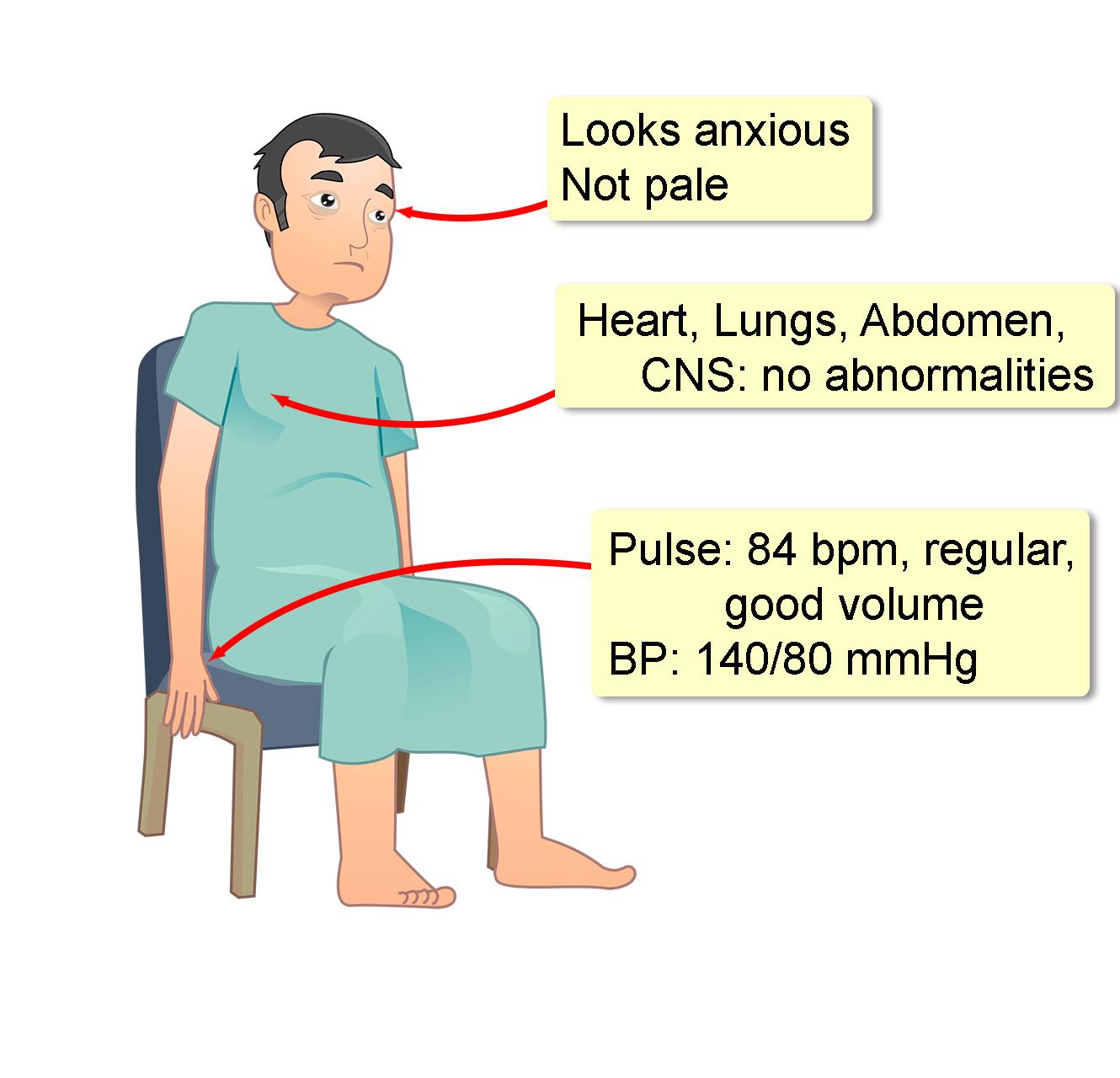
A 50-year-old man presents to the emergency department 20 minutes after he developed severe retrosternal chest pain radiating to the jaw, neck, and left arm. The pain was sudden in onset. At the time the pain started, he was sitting on a chair, watching television. First responders obtained an ECG. This showed ST-segment elevations in leads II, III, and AvF. He was then started on aspirin and sublingual nitroglycerin. By the time of arrival at the emergency department, the chest pain had subsided completely.
His medical history is unremarkable. His most recent routine health screening was 3 months ago. At that time, his fasting plasma glucose and lipid profile were both found to be normal, while his blood pressure measured 130/80 mmHg. His surgical and family histories are also unremarkable. He is not on any routine medications, including over-the-counter drugs or supplements. There is no history of allergies. A complete blood count and chest x-ray are both normal.