Occult 2
1
View details
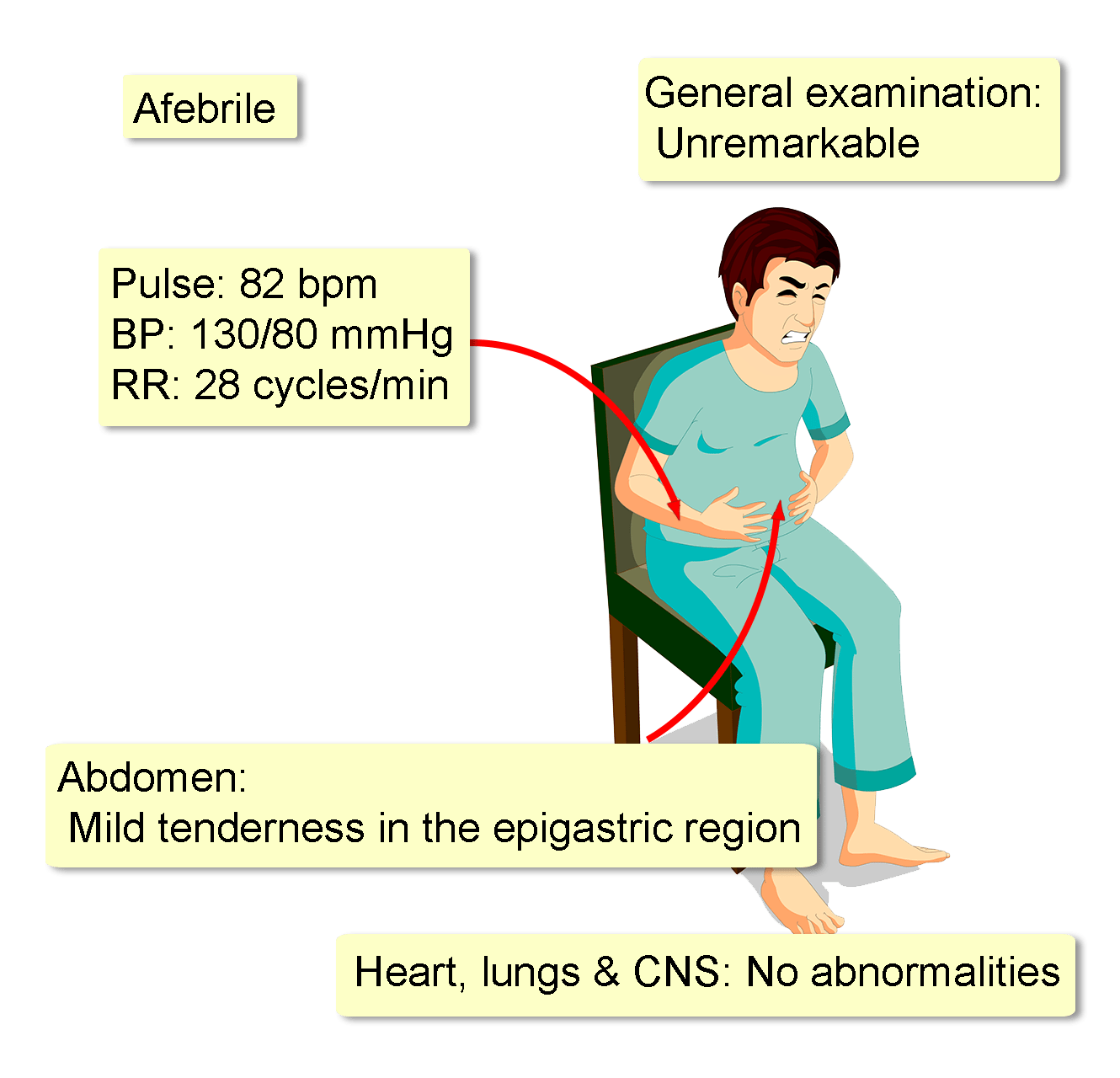
A 43-year-old man presents with severe epigastric pain, nausea, and vomiting for two hours. There is no history of fever, dyspnea, or chest pain. His medical history is significant for type 2 diabetes mellitus diagnosed four years ago. He is currently on insulin therapy due to inadequate control with oral hypoglycemics. His last HbA1C was 7.2%. His surgical history is significant for an episode of acute pancreatitis a year ago. At that time, ultrasound of the abdomen showed multiple gallstones in the common bile duct and gallbladder. He was managed conservatively and refused further endoscopic or surgical treatment. His family history is unremarkable. There is no history of allergies.
Serial ECGs are unremarkable, with no dynamic changes. Ultrasound of the abdomen shows no new abnormalities. A complete blood count is significant for a WBC of 16,000/mm3 (normal: 4,600-11,000). His random plasma glucose is 480 mg/dL (27mmol/L).