Shocking
1
View details
A 54-year-old woman presents to the oncology clinic with a 2-week history of progressively worsening lower back pain radiating down her left leg. She was diagnosed with stage III invasive ductal carcinoma of the breast 3 years ago and completed adjuvant chemotherapy and radiation therapy at that time. She is currently on maintenance aromatase inhibitor therapy. She describes the back pain as a deep ache, rated 6/10, while the leg pain is sharp, shooting, and “electric” in nature, rated 8/10. The pain is exacerbated by movement and coughing. She reports difficulty sleeping due to the pain. Her current analgesic regimen consists of acetaminophen 1000 mg every 8 hours and ibuprofen 400 mg every 8 hours, which provides minimal relief. She denies bowel or bladder incontinence, saddle anesthesia, or recent trauma. She has no known drug allergies.
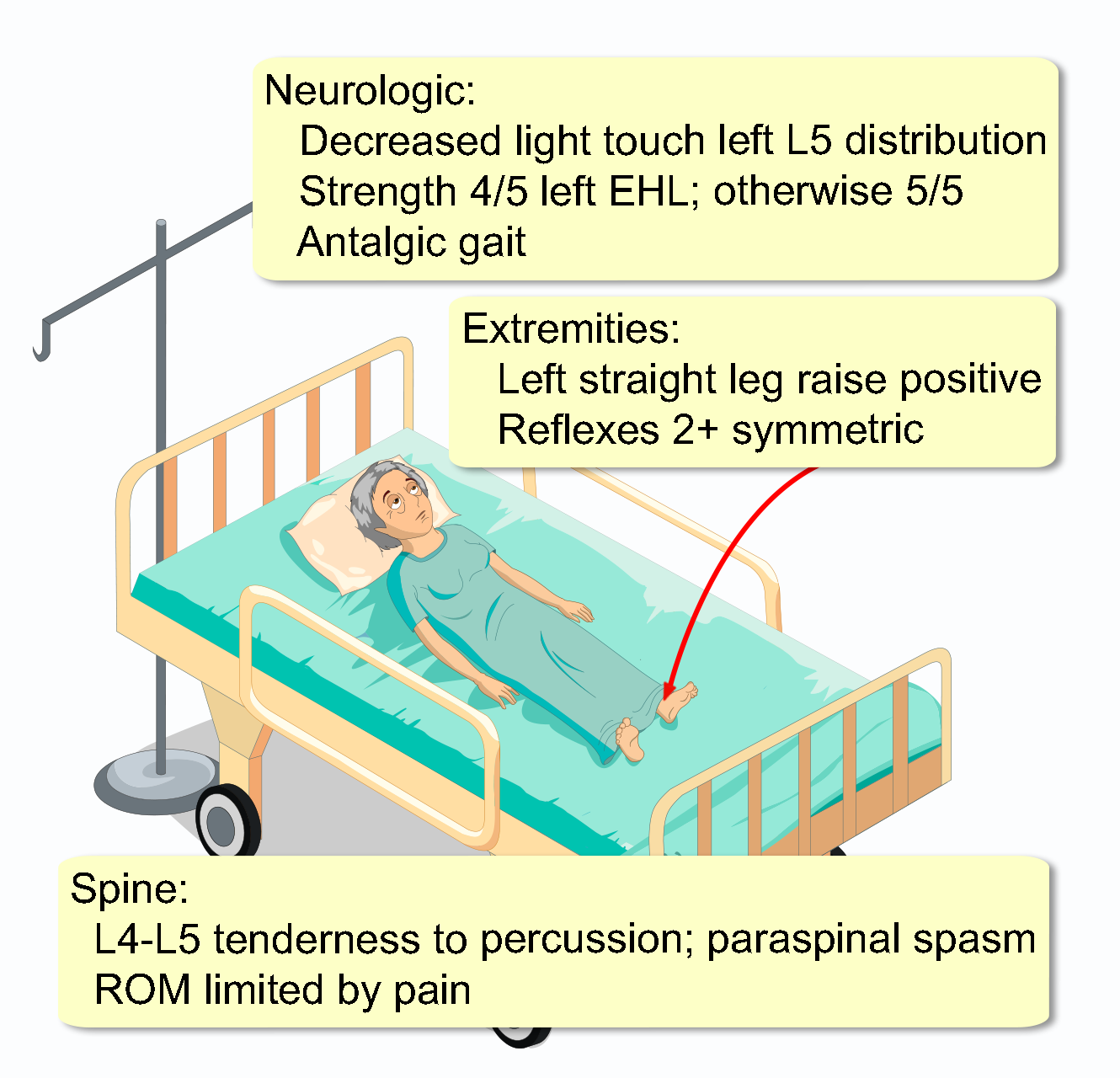
She appears uncomfortable, shifting position frequently in the chair, and grimaces when standing up. She is afebrile. Her blood pressure is 138/84 mmHg with a heart rate of 88 bpm. Her respiratory rate is 18 breaths/min with an oxygen saturation of 98% on room air.