Tangled
1
View details
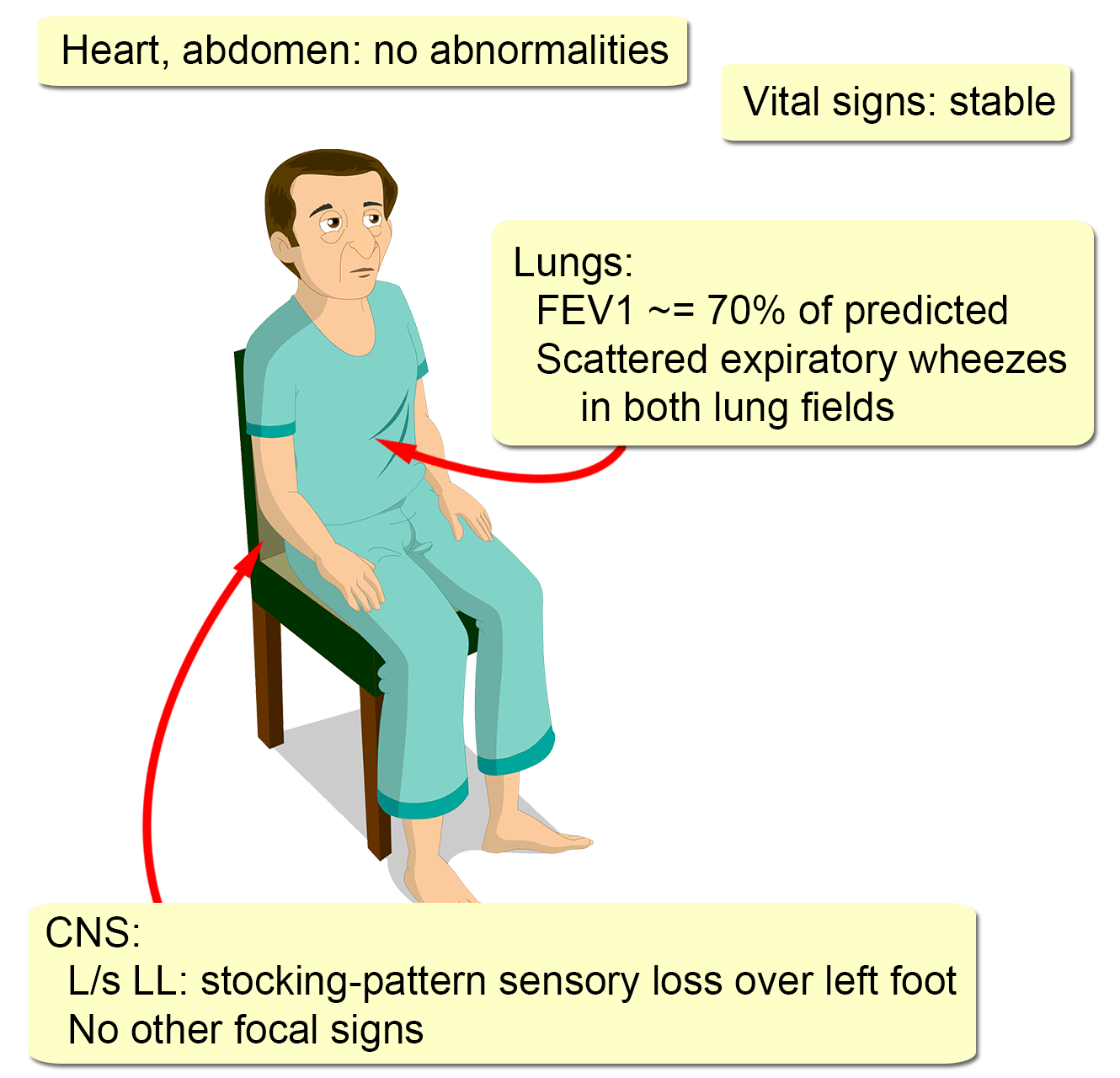
A 42-year-old man presents with tingling and numbness of his left foot for 2 months, in a background of anorexia, malaise, and a 13 kg weight loss over 3 months.
He was diagnosed with infrequent intermittent asthma 11 years ago. This has slowly worsened to moderate persistent asthma, despite good compliance and proper inhaler technique. He has also had allergic rhinitis for the same period.
He is currently on salmeterol, budesonide, and montelukast metered dose inhalers, and occasionally uses over-the-counter anti-histamines. There is no history of allergies to food or medications. He only drinks socially, has never smoked, and denies using recreational drugs.
A complete blood count is significant for leukocyte count of 11,000/mm3 (normal: 4,600-11,000), with 15% eosinophils (normal: 0.0-0.6). A follow up peripheral blood smear confirms hypereosinophilia.
A fasting plasma glucose and HbA1c are both within normal parameters. Liver and renal profiles are within normal parameters. Plain radiographs reveal ill-defined, patchy infiltrates in both lungs.